
Wisdom Teeth
Wisdom teeth are a third set of molars at the very back of the mouth. They're the last teeth to come in, usually emerging in someone's late teens or early 20s. Many people don't have enough room in their mouth to accommodate them and removing them can prevent a number of oral health issues like pain, inflammation, infections, impaction of other teeth, decay of otherwise healthy 2nd molars, and gum disease.


Don't Wait for Pain to Make the Call
Through imaging, we can often see how a person’s wisdom teeth are developing before they erupt, catching any early signs that issues are likely to arise. The earlier we discover these problems the easier the procedure and recovery process are.



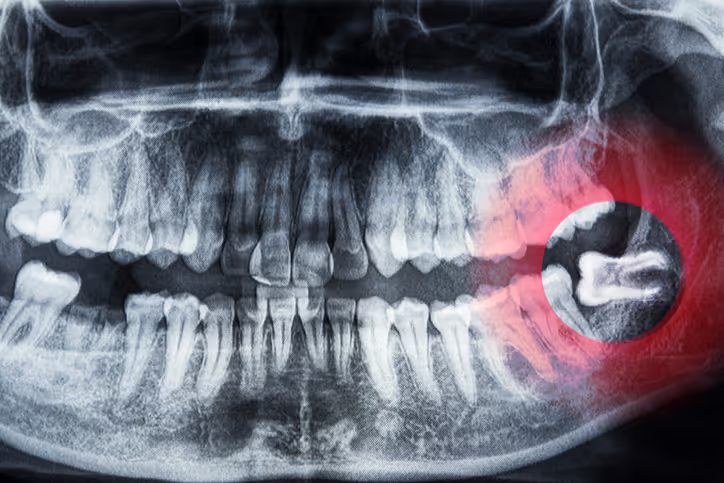


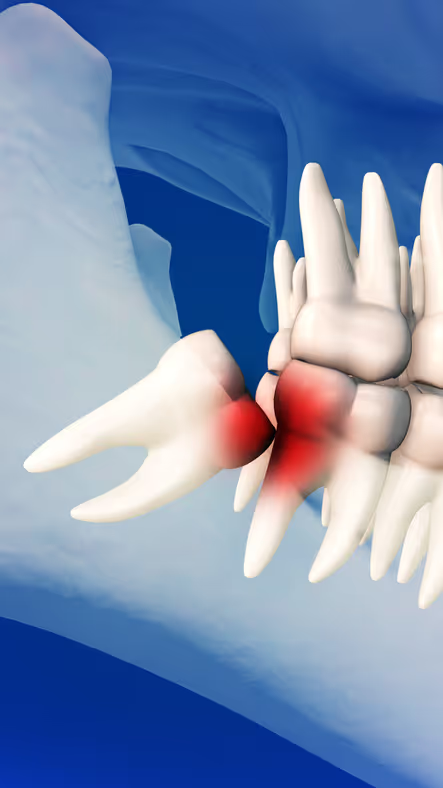

At a Glance
Get in TouchWhat Wisdom Tooth Removal Can Do For You
It's best to get your wisdom teeth removed before they cause problems. Through imaging we can see how the teeth are developing and see if removal is necessary, saving you from issues like infection, damage to your nearby teeth, and pain/swelling in the back of your mouth.
Recovery Snapshot
Most patients have a smooth recovery and describe the pain as minimal. Pain is typically managed with non-narcotic medication and you'll go home with clear instructions for pain control, eating, and hygiene.
Who’s it For?
Anyone that has third molars can benefit from a screening. Some studies have shown that 85-90% of wisdom teeth are ultimately recommended for removal. Getting a screen in your late teens or early 20s is critical for determining if removal is necessary.
Next Step
Even if your wisdom teeth aren't causing you issues now, it's important to get an evaluation and imaging in order to see exactly how your wisdom teeth are developing.
Comfort Options
We have a variety of sedation options from nitrous oxide to IV sedation. All patients will also receive local anesthesia to ensure there's no pain at the surgery site.

Why Remove Your Wisdom Teeth?
Wisdom teeth are the last teeth to come in, and many people’s mouths aren’t big enough to accommodate them. When a person’s wisdom teeth try to erupt in a crowded environment, you can experience issues ranging from impaction (stuck under the gum), to partial eruption, to eruption at an angle that puts pressure on nearby teeth and creates a difficult area to keep clean. Over time, this can even lead to cavities on the 2nd molars, which if the damage becomes severe enough, could require the 2nd molars to be extracted as well.
For some patients, there are signs that signal they could need an extraction, whether that’s pain, swelling, infection, or discomfort when chewing. For others, pain hasn’t become part of the equation yet, but imaging shows there could be problems down the line if the wisdom teeth continue to develop without intervention. Getting imaging early, and taking preventative measures before your wisdom teeth cause pain or infection is critical to avoiding complications.
The goal of wisdom tooth removal is to mitigate future risk and restore comfort to a person’s mouth. By getting an evaluation and imaging before you’re experiencing pain, you can set yourself up to make a proactive and educated decision of whether to get your wisdom teeth removed or simply monitor the situation as it evolves.

When Wisdom Tooth Removal is Recommended
You may be a candidate for wisdom tooth removal if:
- Your wisdom teeth are impacted (stuck under your gum) or only partially erupted.
- You’re experiencing pain, swelling, infection, or discomfort while chewing.
- Your wisdom teeth are coming in at an angle, putting pressure on molars in front of them.
- Imaging shows that your wisdom teeth are creating an environment where you are likely to experience issues such as decay, gum disease, or damage to nearby teeth.
- You’re experiencing a condition called pericoronitis where the gum tissue surrounding the wisdom tooth becomes inflamed. This often happens when excess gum tissue is irritated by chewing, food getting trapped beneath the gum, or plaque building up in the area and calcifying.
If you’re unsure if you fall into one of these categories, request a consultation and we can help you get some clarity!


What is Dry Socket?
Dry socket or alveolar osteitis is a post-extraction complication that occurs when the normal blood clot in the extraction socket is lost or fails to form, exposing underlying bone and nerve endings.
Symptoms may include:
- Severe throbbing pain starting 2–4 days after extraction.
- Pain that radiates to the ear, temple, or neck.
- An unpleasant odor or taste.
Dr. Seda uses special techniques, and materials to avoid the incidence of dry socket. He’ll also carefully review post-operative instructions with you to ensure you follow a regimen that protects the healing site.
To help prevent dry socket, patients are advised to avoid using straws, spitting, and smoking for 2 weeks after extraction.
If dry socket does occur, an intrasocket medication can be placed to reduce pain as it heals.


The Seda Approach Step By Step

